Varicoceles

Varicoceles
98% success rate, with no groin incisions
WHAT ARE VARICOCELES AND HOW COMMON ARE THEY?
Varicoceles are enlarged varicose veins around the testicle that can cause pain, swelling, and infertility. This condition affects 15 out of 100 men overall and 40 out of 100 men with known infertility.
A varicocele develops due to poorly functioning valves in veins, causing blood to flow in the wrong direction, and increasing the pressure within the vein. Varicoceles are most often identified in young men but can occur at any age.
Varicoceles can cause pain, testicular swelling (may feel or look like a bag of worms), low sperm production, and decreased sperm quality, leading to infertility. In younger males, varicoceles are repaired due to fertility concerns.
WHAT ARE THE SYMPTOMS OF A VARICOCELE?
Varicoceles cause infertility and/or pain. The pain may:
- Vary from sharp to dull discomfort in the groin or testicular area
- Increase with standing or physical exertion, and heavy lifting
- Worsen over the course of a day
- Be relieved when you are lying down
Varicoceles over time may cause testicular atrophy and cause infertility.
HOW ARE VARICOCELES DIAGNOSED?
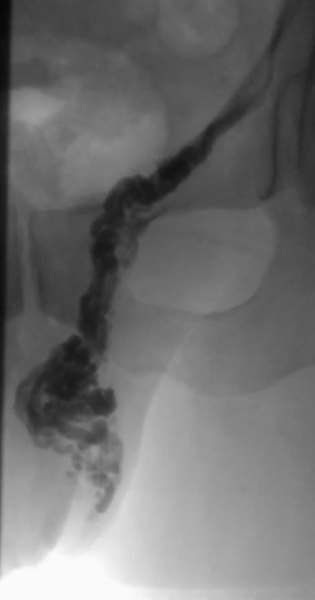
Varicoceles cause testicular swelling, and when significant, appear like a bag of worms in the scrotum. However, there are many causes of testicular swelling, and an ultrasound examination is the best way to identify and classify a varicocele.
WHAT SHOULD I DO IF I WAS DIAGNOSED WITH A VARICOCELE?
If you have testicular or groin pain, eliminating the varicocele is very effective at improving or eliminating pain. In younger males who desire fertility, elimination of the varicocele should be considered to prevent testicular atrophy and infertility. If you have no symptoms or fertility concerns, no treatment is required.
WHAT ARE THE TREATMENT OPTIONS FOR A VARICOCELE?
WHAT WE DO:
- Varicocele embolization: a tiny incision is made, and a catheter is guided into the veins supplying the varicocele. The non-functioning veins allowing blood to leak into the varicocele are closed using tiny metal coils, and the blood then drains out of the testicle through normal veins.
WHAT WE DON'T DO:
- Open surgery (varicocelectomy): open surgery to ligate (cut) varicocele veins.
IS VARICOCELE EMBOLIZATION SUPERIOR TO SURGERY?
Both surgical and embolization techniques work well. However, outcomes largely depend on the skill of the person performing the procedure.
Varicocele embolization has several advantages over surgery, including:
- No large incisions
- Less post-operative
- Faster recovery
- Lower complication rates, especially infection
- No general anesthesia
Dr. Cumming specializes in varicocele embolization. In his experienced hands, he has a 98% success rate of treating and embolizing the varicocele. In 94% of these patients, venous reflux was entirely resolved, and the varicocele disappeared. In addition, 80% of the patients reported complete resolution of their testicular pain.
WHAT ARE THE BENEFITS OF VARICOCELE EMBOLIZATION?
- Higher success rate of fixing a varicocele
- Eliminates pain stemming from a varicocele
- Improvement of the quality of sperm in about 50% of patients
- Much lower overall risk than conventional surgery
- No surgical incision in scrotal area
- As effective as varicocele surgery at improving semen analysis and pregnancy rates
- Patients can return to normal daily activities immediately
- No required hospital admittance
- Varicoceles occuring on both sides can be fixed simultaneously through one vein puncture site
- No general anesthesia required
- No sutures
- Reduced chance for infection
- Varicocele repair improves testosterone and sexual function, including erection and ejaculatory functions1.
Can varicocele embolization improve male fertility?
Yes, according to a recent study, varicocele repair, including embolization, improves male fertility outcomes2. Regardless of prior semen analysis results, patients who underwent varicocele repair saw increased likelihood to achieve pregnancy and live birth.
Additionally, patients who treated their varicocele had better results with sperm retrieval, suggesting that it is beneficial to treat a varicocele before beginning or continuing any fertility program.
HOW IS VARICOCLE EMBOLIZATION PERFORMED?
Through a small incision, a catheter is guided into the veins supplying the varicocele. Then, the abnormal veins are eliminated through a procedure called embolization. The procedure typically takes less than 45 minutes, in a comfortable setting. Patients typically return to work or school the next day and are often back to complete normal activity within a couple of days.
AM I A VARICOCELE EMBOLIZATION CANDIDATE?
If you are experiencing pain caused by your varicocele, have infertility issues due to low sperm count or abnormal sperm, or have future fertility concerns, you are a candidate for this highly safe, effective, and minimally invasive procedure.